Advances in neurostimulation with improved outcomes and reduced invasiveness have challenged the traditional algorithms for pain management. Traditional pain management algorithms previously favored nerve blocks followed by radiofrequency ablation (RFA) prior to considering neurostimulation implants as an option.
Recent innovations provided by temporary percutaneous peripheral nerve stimulation (PNS) treatment have led interventional pain specialists to ask, “What type of pain treatment do back pain patients prefer when they are appropriately informed of the risks and benefits?”
A team of leading interventional pain management specialists, a medical ethicist, and researchers from SPR Therapeutics, Inc., recently launched a project to answer this question. The project involved two surveys. The first survey (n=129) focused on patient preferences involving temporary treatments versus permanent implants while the second survey (n=347) focused on understanding the specific preferences regarding the two most highly preferred treatments from survey 1: Temporary PNS versus RFA. Conservative treatments such as blocks or injections were not considered as they are typically exhausted before considering more advanced or invasive treatments.
“This is the first known survey of its kind,” Dr. Amit Gulati, lead researcher and President of World Academy of Pain Medicine United said. “We sought to characterize patient preferences from among the various interventional pain management options available today to better understand how patients receive these potential treatment options when they are well-informed about the pros and cons of each.”
From the survey results, Gulati, et al., concluded patients prefer temporary PNS as a first-choice interventional treatment for low back pain. The results also highlighted key areas in which physicians can better assist patients in the treatment-selection decision making process especially regarding clearly calling out the potential for adverse events such as multifidus denervation associated with RFA and the potential for fracture of the temporary PNS lead.
Temporary PNS Preferred Over RFA and Permanently Implanted PNS, SCS and DRG
The first survey revealed an overall preference for temporary percutaneous PNS among all respondents.See Graphic 1 below.
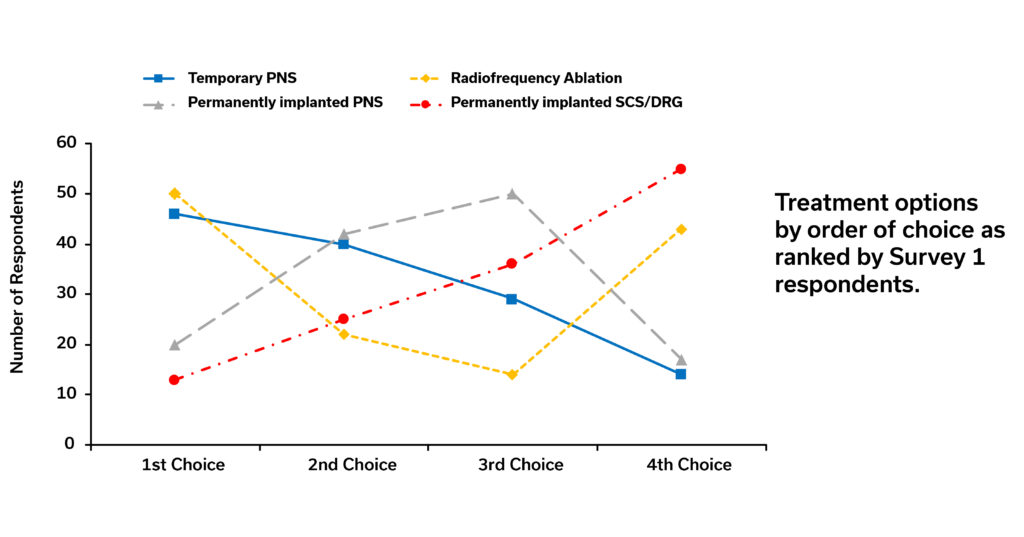
Graphic 1
Graphic 1 shows that most respondents ranked either RFA or temporary PNS as their first-choice option. Mean ranks (see Graphic 2 below) were also calculated by awarding scores (e.g., 4 points for first choice, 3 points for second choice, etc.) to consider the overall preferences of patients across the full range of options. Temporary PNS had, on average, the highest mean rank score, meaning it was overall the most preferred treatment option by patients. Surveyed patients next choice was RFA, while permanently implanted SCS (spinal cord stimulator) or DRG (dorsal root ganglion) systems were least preferred overall.

Based on the mean rank scores by treatment option, Survey 1 revealed the following insights about patient preference for temporary PNS:
- Overall, patients prefer PNS more than RFA and permanently implanted SCS/DRG/PNS.
- Temporary PNS ranks as a top choice for patients suffering from chronic pain.
Low Back Pain Patients Surveyed Preferred Temporary PNS Over RFA
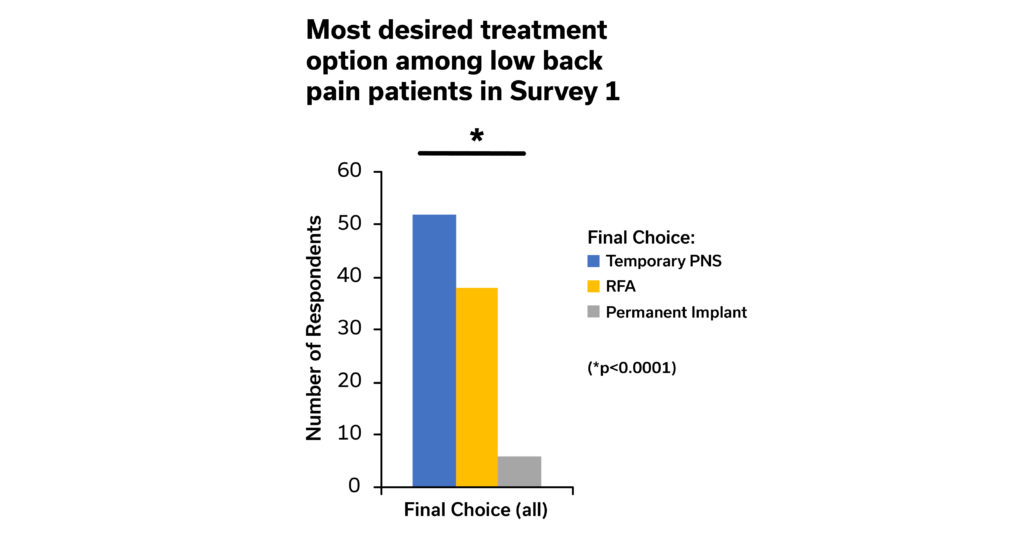
Patients that initially chose temporary PNS or RFA as their top choice were then presented with additional information about the risks of temporary PNS (i.e., the potential for lead fracture) and RFA (i.e., the potential for denervation of multifidus muscle). Afterwards, they were asked to select a final preferred treatment option. The “final choice” treatment in Graphic 3 above reflects the preferences of patients after considering the risks of the temporary PNS and RFA procedures. Low back pain patients surveyed indicated that temporary PNS was the most desired treatment option for treating back pain. RFA was the second most desired option, and a small percentage of patients changed their preference to permanently implanted SCS/DRG/PNS after receiving additional information about risks of temporary PNS and RFA. (See Graphic 3).
Temporary PNS is Most Desired Low Back Pain Treatment Method Among Survey Respondents
Survey 2 provided further insights into the overall treatment preferences of a second set of low back pain patients by offering survey respondents the following options: stimulation, ablation or neither. The surveyed patients were provided with a description of each treatment option, as reviewed and co-drafted by a medical ethicist, to explain pros and cons of each treatment as accurately as possible. Like Survey 1, patients were provided with additional information about the risks of each treatment option and then asked to select a final preferred treatment option.
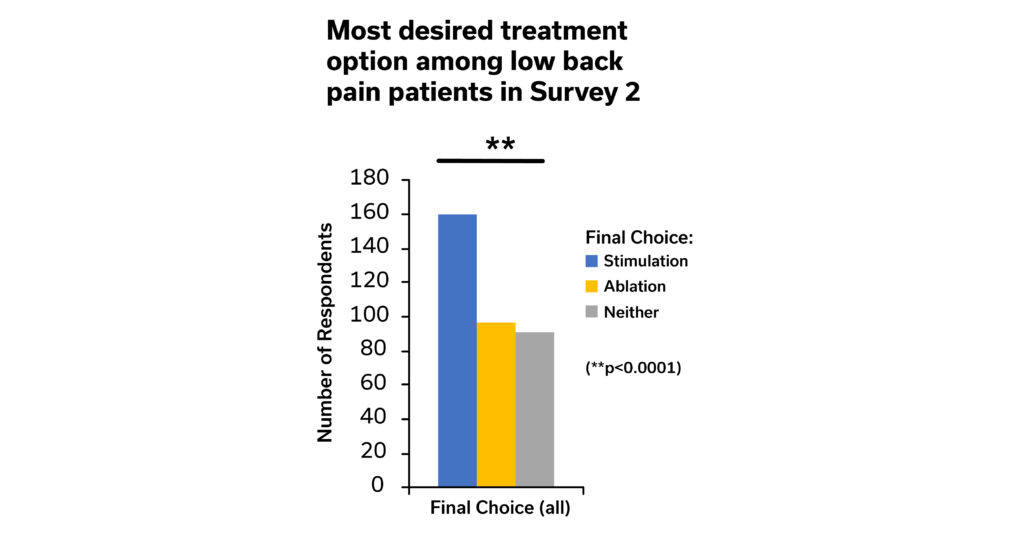
In Graphic 4 below, Survey 2 respondents indicated that stimulation was most desired over ablation, where “stimulation” equates to the SPRINT PNS System and 60-day PNS procedure, while “ablation” refers specifically to radiofrequency ablation. Among those that preferred an intervention (i.e., excluding those that selected “Neither”), 62 percent of respondents preferred 60-Day PNS while only 38 percent preferred radiofrequency ablation.
These data further confirm Survey 1 results indicating that patients who are informed about the potential benefits and risks of temporary PNS and RFA tend to prefer temporary PNS over RFA for treating back pain.
Patient Preference Findings Highlight Opportunities for Physicians to Better Help Patients in Making Informed Decisions
“The above findings in this research lend key insights into the value of temporary PNS and peripheral nerve stimulation overall, but they also spotlight where physicians can better assist their patients,” co-author Mark Stultz, PT, said. “New interventional pain management treatment options have resulted in improved outcomes and reduced invasiveness, but they’ve also brought the challenge of characterizing these options in a way that fosters optimal patient understanding and participation in treatment selection.”
In addition to insights about patient preferences, these surveys revealed important lessons about ethically communicating treatment options, potential benefits, and risks to patients to help inform their choices.
The following are key takeaways for patient-centered physicians to consider when working with chronic pain patients:
- Verbal descriptors are important when seeking to help patients evaluate their treatment options
- Ensure treatment descriptors are accurate, clear and don’t accidentally mislead patients
- Present patients with a clear understanding of each treatment’s potential for efficacy as well as adverse events
In the end, it’s clear from the above results that a patient’s preference and understanding of available treatment options are important considerations when determining a pain management treatment plan.
Further Reading: Temporary PNS Multi-Center Study Demonstrates Sustained Relief in Low Back Pain Patients
The above results, which indicated a preference for temporary PNS over RFA and permanently implanted PNS, SCS or DRG, are not surprising to see given the results of another recent study reviewing temporary PNS in a multi-center trial in patients with low back pain.
Recently published by PAIN Practice (July 2021), read “Treatment of Chronic Axial Back Pain with 60-day Percutaneous Medial Branch PNS: Primary Endpoint Results from a Prospective Multicenter Study,” for further insights into the clinical evidence for temporary PNS.

 SPR Therapeutics CEO Maria Bennett Selected as Winner of EY Entrepreneur of the Year in East Central Region
SPR Therapeutics CEO Maria Bennett Selected as Winner of EY Entrepreneur of the Year in East Central Region

Leave a Reply