
Are stress and pain related? Which is the chicken and which the egg? Can the one lead to the other?
According to a 2017 study published on the National Center for Biotechnology Information website, the answer is yes. The study identifies two models connecting pain and stress.
- Model 1: Pain is a type of stress that adds strain to an organism which in turn results in stress increasing pain and pain perception.
- Model 2: Unpredictable stress triggers pain that leads to a cycle of maladaptive physiological responses (e.g., inflammation, brain damage) that thus increases vulnerability to persistent pain.
In simpler terms, stress and pain can exist simultaneously, cause one another, and result in decreased well-being. Furthermore, they often exacerbate each other.
In August 2020 a new study proposed that chronic pain is complex and should be evaluated in the context of numerous interacting factors including biological, psychological and social. It also noted that chronic pain could be triggered by psychosocial stressors.
The above research begs the question: has the COVID-19 pandemic indirectly caused increased levels of pain and/or patients with pain?
Stress during COVID can lead to increased chronic pain
The pandemic caused and worsened a number of psychosocial stressors. Limited interpersonal contact, financial strain, sustained unemployment, fear of illness and death, constant media coverage full of conflicting information, isolation, and figuring out at-home work and education situations are just some of those stressors.
According to a poll conducted between April and May 2020 by the American Psychological Association, the average reported stress level for adults in general was 5.4, and in relation to COVID specifically, 5.9 (on a scale of 1 to 10, where 1 means “little or no stress” and 10 means “a great deal of stress”). During same timeframe for adults with children under the age of 18 the average stress level was 6.7, with nearly half of parents saying their stress level was high (between 8 and 10 on the 10-point scale).
In February this year, an article by the Anchorage Daily News reported that local clinicians were seeing increased numbers of patients with “posture- and stress-related pain” over the last year, including increases in back and neck pain as well as headaches. But what one clinician said he found most concerning was the “increased levels of pandemic-related stress and anxiety.” The article goes on to observe similar stress increases in children and adults, and that when stress is not relieved it can manifest physically, such as muscle spasms or dehydration.
Discussing Observations of Stress and Chronic Pain with Dr. Mehul Desai
In looking at the last year and the chronic stress experienced by many, we wondered if interventional pain physicians had observed similar things, including a link between stress and pain. In March, we sat down with Dr. Mehul J. Desai, Chief of the Division of Pain Medicine at Virginia Hospital Center, President of International Spine, Pain & Performance Center, and Clinical Assistant Professor at The George Washington University School of Medicine and Health Sciences. Read below to hear what Dr. Desai observed in the last year, as well as to get some helpful tips Dr. Desai has used with his own patients suffering from pain.
SPR: Since the pandemic started, what have you observed in your patients in terms of stress and chronic pain?
Dr. Desai: It’s been very interesting; we are seeing sky-high stress levels even in a city that is chronically stressed like Washington DC. The sense of isolation and uncertainty seem to be responsible for these stress levels and the stress levels have pushed pain levels upward. Patients are reporting lower pain tolerance and a sense of hopelessness that is very concerning.
SPR: So, it sounds like you’ve seen similar results to what was reported in the Anchorage article – increases in both stress and pain. Do you have any proposed theory for why chronic pain patients specifically may have seen increased pain levels?
Dr. Desai: So, there are a few things that likely led to this. First, we know that there is a relationship between stress and pain and that stress seems to make pain worse. The pandemic clearly created a highly stressful environment around the world, one that significantly worsened chronic stress.
Second, the pandemic caused an enormous amount of isolation. Normal coping patterns were disrupted. Friends, exercise, religion were all affected and access to them was limited. The amount of internalization this caused tended to be unhealthy as there were few other issues to focus on.
Finally, due to the need for social distancing and the uncertainty around COVID-19, the pandemic likely altered what treatment options were available to many patients. Interestingly, patients seem to look forward to their telehealth appointments, both to address their health conditions but also to stay connected. We found ourselves focusing on primarily on psychosocial issues during telemedicine appointments and helping patients create healthy outlets and strengthen their coping strategies.
SPR: You mentioned a “sense of hopelessness as one of your observances. Can you explain what you mean by that?
Dr. Desai: Well, I think a better way to think of this is via a group of concepts including negative outlook, hopelessness, and catastrophizing. Often patients dealing with chronic pain suffer from these issues at baseline and it is very clear that the pandemic worsened these. Basically, the inability to shift focus away from pain and negative stressors work to make the pain worse. The lack of normal coping patterns heightened this. Catastrophizing is when folks have the tendency to look at any situation through a negative lens and to make situations seem worse than they are. This was often the case during the pandemic.
It is very difficult to remain patient when dealing with pain. Hope is another necessary element here, and the coping methods I mention above often help with this – again because they allow the patient to shift focus away from the pain and towards something positive. This shift helps creates hope; hope for a healthier lifestyle and potentially a pain-free future.
Even for those folks with good coping skills, being affected by COVID-19 and having limited access to normal treatments can make it difficult to maintain a positive outlook. It’s sort of a doubling effect here, where the mechanisms that a patient usually leverages to cope with pain or improve it are no longer there, and then the treatments a patient needs are limited or altered. Drop a third element into the mix, the constant media stream of bad news, and a sense of hopelessness can become overwhelming.
SPR: With the impact of the pandemic, what were (and are) your recommendations for helping individuals to combat pain?
Dr. Desai: I try to change the way we frame these conversations. We talk to folks about managing their pain but also reducing their stress. The biggest thing is be open to new ways of engaging yourself – new opportunities to explore and activities to do that maybe you didn’t have time for previously. For example, maybe your job required you to be stuck in an office for eight hours straight. Now you’re working from home, so take advantage of that by blocking off small sections of time where you could take a short nature walk, or if you can, set up your office outside if the weather is nice. Getting outside, enjoying the fresh air, even just a quick walk, or sitting outside – the goal is to shift your focus away from the pain.
I’d also recommend that people be open to new treatment options they may not have been inclined towards before. Open yourself to idea of virtual treatment and telemedicine. There are lot of terrific free apps that help with mindfulness and diet. Take on new hobbies if able. Focus on things maybe you didn’t have the time to focus on previously like nutrition. Instead of thinking things are stressful because your traditional treatments options aren’t accessible now, try instead to focus on the unique benefits you can get with telemedicine. Telemedicine is often more flexible and may not impact your schedule as much. It may not be the same as in-person, but it’s still better than none.
SPR: Those are all great recommendations. Is there anything else that you think people should take away when considering how to handle chronic pain, and also chronic stress, right now?
Dr. Desai: Absolutely, we want to make sure that the options we offer patients are robust and not one-dimensional. We are continuing to innovate, educate and communicate. The silver lining of COVID-19 is that it forced us to evolve. Patients are our partners in their treatment, each plan should be individualized.
About Dr. Mehul Desai
Mehul J. Desai, MD, MPH, is the Medical Director of the International Spine, Pain & Performance Center and Chief, Division of Pain Medicine at Virginia Hospital Center. A board-certified physician, Dr. Desai provides comprehensive care using cutting-edge technologies for a number of pain conditions. He has received extensive training in pain medicine and physical medicine and rehabilitation, and in addition to his roles mentioned above, he also holds the following titles and responsibilities: Director, Interventional Spine and Musculoskeletal Medicine Fellowship (NASS); Medical Director, the Performance Lab; President, Monument Research Institute; and Clinical Assistant Professor, Department of Anesthesiology & Critical Care, George Washington University, School of Medicine.

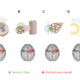 Could 60-Day Percutaneous PNS Treatment Lead to Sustained Pain Relief by Reconditioning the CNS?
Could 60-Day Percutaneous PNS Treatment Lead to Sustained Pain Relief by Reconditioning the CNS?

Leave a Reply